Apr 2016
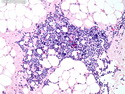
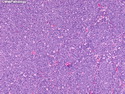
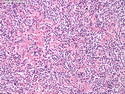
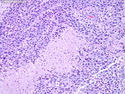
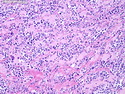
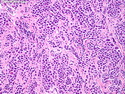
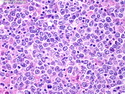
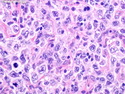
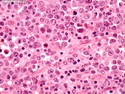
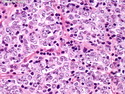
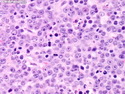
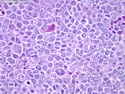
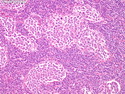
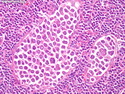
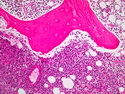
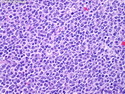
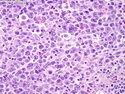
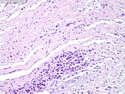
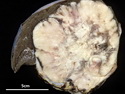
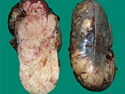
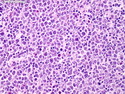
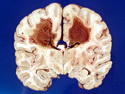
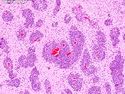
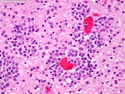
Diffuse Large B-cell Lymphoma
Reviewer(s): Dharam M. Ramnani, MD
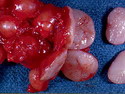
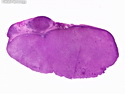
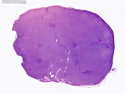
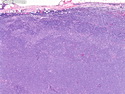
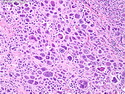
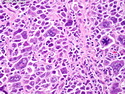
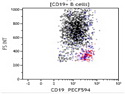
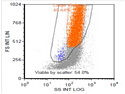
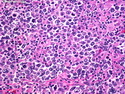
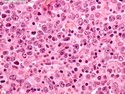
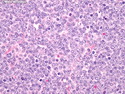
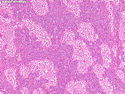
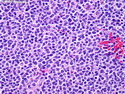
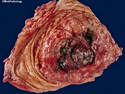
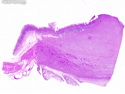
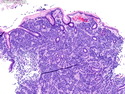
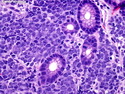
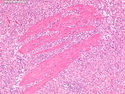
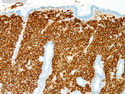
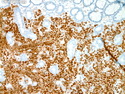
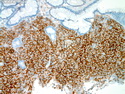
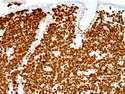
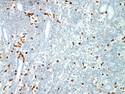
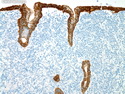
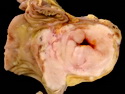
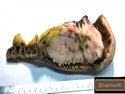
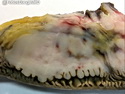
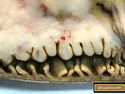
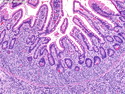
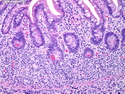
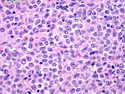
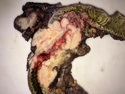
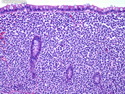
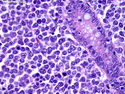
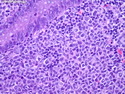
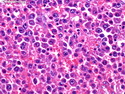
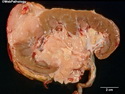
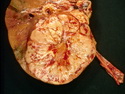
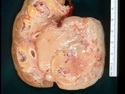
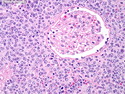
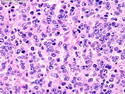
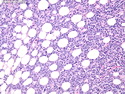
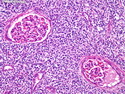
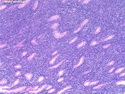
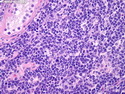
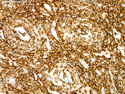
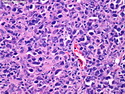
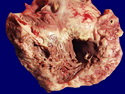
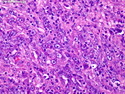
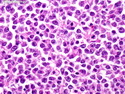
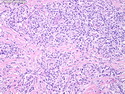
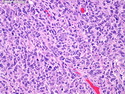
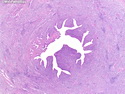
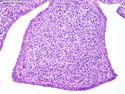
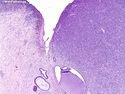
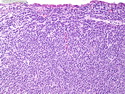
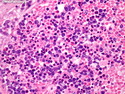
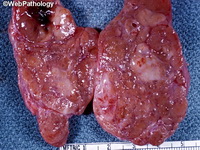
Diffuse large B-cell lymphoma (DLBCL) is the most common type of non-Hodgkin lymphoma accounting for about 30% of all cases. It is an aggressive malignancy and is seen mostly in adults (median age 64 years). Patients present with rapidly enlarging lymph nodes or tumor masses (extranodal sites). Extranodal sites are commonly involved (almost 40% of cases) and include gastrointestinal tract, central nervous system, skin, mediastinum, and bone, but any organ can be involved. Bone marrow and liver involvement is less frequent than in follicular lymphoma or small lymphocytic lymphoma. Morphology: The cut surface of involved lymph nodes or tissues is soft and fleshy with effacement of the native architecture. There is diffuse proliferation of large to medium-sized lymphoid cells which can be classified into following subtypes: 1) Centroblasts - round, angular, or multilobated vesicular nuclei; multiple small peripheral nucleoli; indistinct amphophilic cytoplasm. 2) Immunoblasts - round or oval vesicular nuclei; single prominent central nucleolus; abundant basophilic cytoplasm. 3) Anaplastic - markedly pleomorphic large tumor cells. Necrosis, numerous mitoses, and starry sky pattern may also be seen. Immunophenotype: DLBCL expresses CD45 and pan B-cell markers such as CD20, CD22, CD79a, and PAX-5. Monotypic immunoglobulin (surface or cytoplasmic) is variably present. Other positive markers include CD10 (40% cases), BCL6 (60% cases), and BCL2 (50% cases). CD5 is present in about 10% of cases. A small number of cases show post-germinal center or plasma cell-associated markers such as CD38, VS38, and MUM1. Ki-67 labeling index is high (>20%). A minority of cases express CD30. Pan-T markers are negative. Molecular genetics: Immunoglobulin heavy- and light-chain genes are rearranged. The immunoglobulin heavy-chain variable region gene is hypermutated. Rearrangements of BCL2 and BCL6 genes are seen in 20% and 30% of cases respectively. MYC (8q24) translocation is seen in about 10% of cases, usually fused to a non-immunoglobulin gene in contrast to Burkitt lymphoma.