Apr 2017
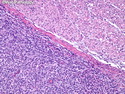
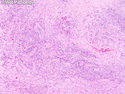
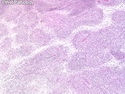
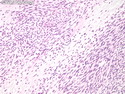
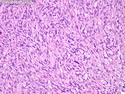
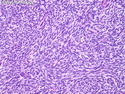
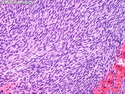
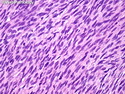
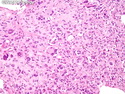
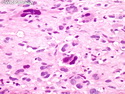
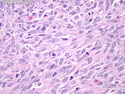
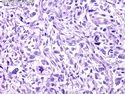
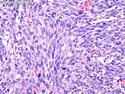
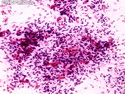
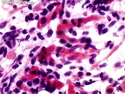
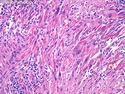
Malignant Peripheral Nerve Sheath Tumor
Reviewer(s): Dharam M. Ramnani, MD
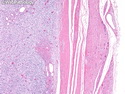
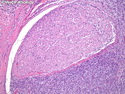
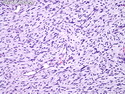
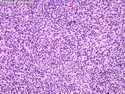
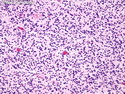
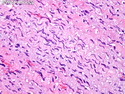
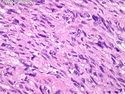
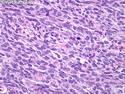
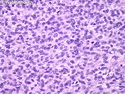
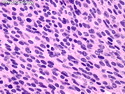
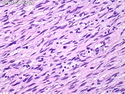
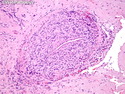
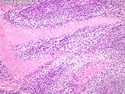
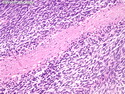
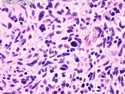
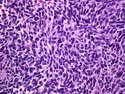
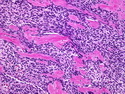
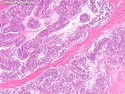
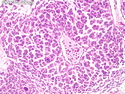
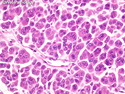
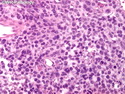
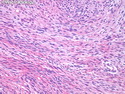
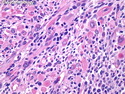
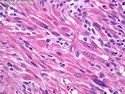
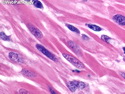
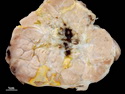
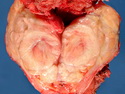
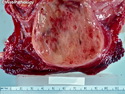
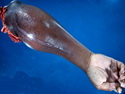
Malignant peripheral nerve sheath tumors (MPNST) are a group of high-grade sarcomas that show differentiation along one of the nerve sheath elements such as Schwann cell, perineural cell, and fibroblast. They make up 5% to 10% of all soft tissue sarcomas. About 50% arise de novo; the remainder in the setting of neurofibromatosis 1 (NF1). They usually occur in adults along one of the major nerve trunks such as sciatic nerve, brachial plexus, and sacral plexus. MPNSTs are large, fleshy tumors and commonly show areas of necrosis and hemorrhage. The diagnosis of MPNST is made if a fibrosarcomatous-appearing tumor : 1) obviously arises from a peripheral nerve; or 2) the tumor arises from a preexisting neurofibroma in NF1; or 3) the tumor has histologic features of a malignant Schwann cell tumor - including hyper- and hypocellular areas, irregular wavy hyperchromatic nuclei with tapered ends, whorled structures, epithelioid appearance of perivascular tumor cells, and immunohistochemical or ultrastructural evidence of Schwann cell differentiation. About 15% of MPNSTs show heterologous elements. The differential diagnosis of MPNST includes fibrosarcoma, monophasic synovial sarcoma, leiomyosarcoma, desmoplastic melanoma, as well as neurofibromas with atypical features. The diagnosis of MPNST is favored by positivity for S-100, nestin, HMGA2, and SOX10.
MPNSTs are high-grade sarcomas with a tendency to local recurrences (about 40% of cases) as well as distant metastases (40% to 60% of cases) after resection. References: 1) Rosai & Ackerman's Surgical Pathology, Tenth Edition, 2011; Chapter 25: Soft Tissues, p. 2137-40. 2) Enzinger & Weiss's Soft Tissue Tumors, Sixth Edition, 2014; Chapter 28: Malignant Peripheral Nerve Sheath Tumors; p. 855-879.


.jpg)