IPMN : Diagnosis

Comments:
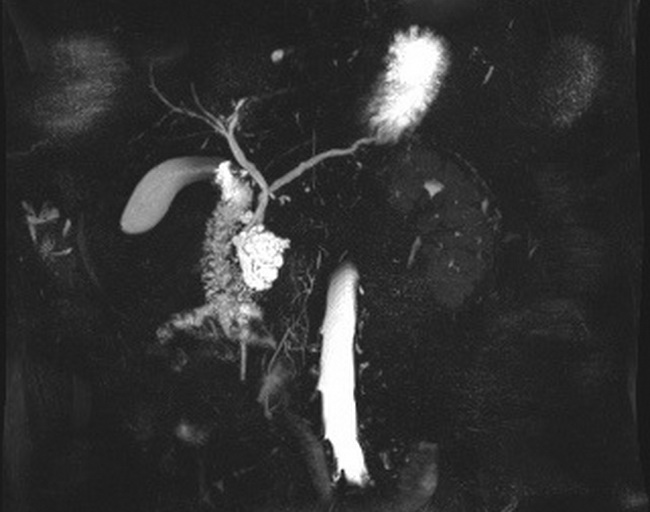
Diagnosis: Intraductal papillary mucinous neoplasms (IPMNs) of pancreas can be detected on imaging using various modalities including computed tomography (CT), magnetic resonance imaging (MRI), or endoscopic retrograde cholangiopancreatography (ERCP). Based on the location seen on imaging studies, IPMNs are categorized as main duct (MD), branch duct (BD), or mixed-type (MD and BD) types. On CT, a MD-IPMN appears as a segmental or diffuse dilatation of the main pancreatic duct. A BD-IPMN involves smaller secondary ducts and is seen as a single cyst or multiple cysts. MRI can show mural nodules or irregularities in the duct contours that are suggestive of higher grade lesions, such as IPMN with HGD or with invasive carcinoma. On ERCP, IPMNs are associated with dilated ducts and filling defects, but the pathognomonic feature is mucin extravasation from the ampulla of Vater into the duodenum (as shown in slide 2). Cyst fluid analysis can be used in conjunction with other modalities to aid in the diagnosis of cystic lesions of the pancreas. IPMNs will have elevated carcinoembryonic antigen (CEA) and amylase, as well as increased viscosity. In contrast, mucinous cystic neoplasm (MCN), a main differential diagnosis for IPMN, will have elevated CEA and increased viscosity, but normal amylase. About this image: MRI with contrast (coronal maximum intensity projection) shows a 1.8 cm multicystic lesion arising from the side branch of pancreatic duct in the head of the pancreas. The lesion can be seen just to the left of the center of this image. It has the classic appearance of a bunch of grapes hanging from a stem. Case courtesy of Dr Ian Bickle, Radiopaedia.org. From the case rID: 59609



