Candida Esophagitis : Diagnosis

Comments:
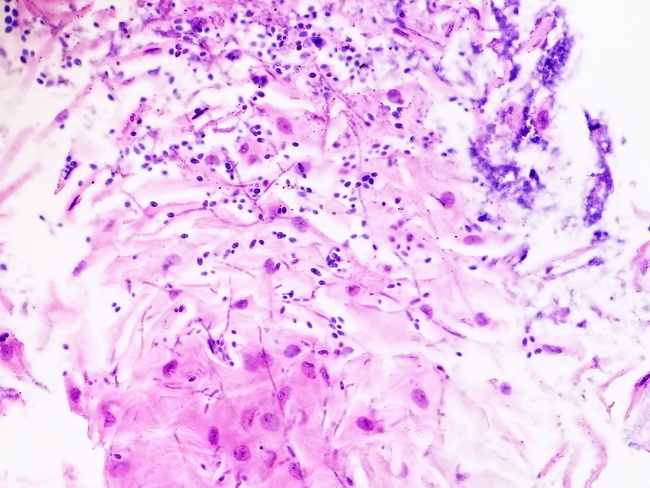
Diagnosis: Patients with candida esophagitis present with dysphagia, odynophagia, and retrosternal pain. Some patients are asymptomatic. Endoscopy shows white plaques or pseudomembranous exudate distributed along the length of the esophagus as shown in the previous image. Ulcers are rare. Before the widespread use of endoscopy, the imaging modality used was double contrast barium esophagography. The diagnosis can be made by brushing the lesion, followed by cytology or biopsy. Esophageal brushings are more sensitive than biopsies. With Papanicolaou stain, the hyphae and budding yeast stain red in a background of inflammatory and squamous debris. Sections show pseudohyphae, true hyphae, and clusters of budding yeast in the superficial layers of acutely inflamed squamous mucosa. Special stains such as PAS or GMS may be required to identify the fungal organisms. Note:: Candida can grow as yeast, pseudohyphae, and true hyphae depending upon the environmental conditions. Yeasts are single cells, ellipsoid to spherical in shape and ranging in diameter from 3 to 15 microns. Pseudohyphae are chains of elongated yeast cells. They result from incomplete budding when the cells fail to detach after cell division and continue to elongate. True hyphae are parallel-sided branching, filamentous or tubular fungal cells, usually separated by porous cross-walls or septa. Image courtesy of: Brian Odum, MD; used with permission.



