MPNST : Differential Diagnosis

Comments:
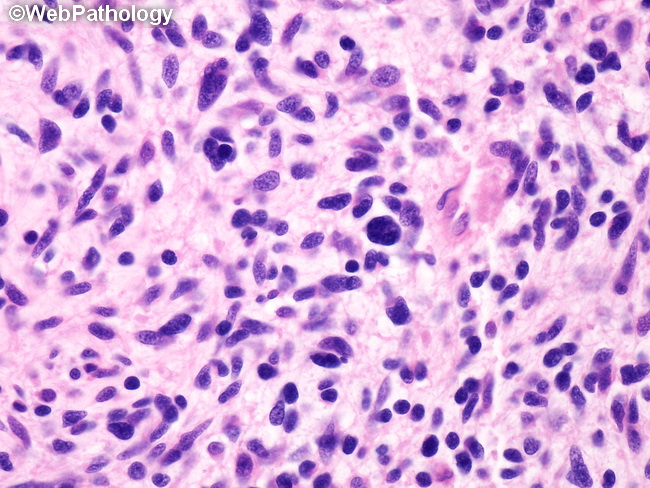
The differential diagnosis of a malignant peripheral nerve sheath tumor includes fibrosarcoma, monophasic synovial sarcoma, leiomyosarcoma, desmoplastic melanoma, as well as neurofibroma with atypical features. Fibrosarcomas and monophasic synovial sarcomas are composed of uniform fibroblastic cells arranged in intersecting fascicles. They lack neural differentiation. Monophasic synovial sarcoma can be confirmed with molecular studies. A reciprocal chromosomal translocation t(X;18)(p11.2;q11.2) resulting in S18-SSX fusion gene is characteristic of nearly all synovial sarcomas. This translocation fuses the SS18T (SYT) gene from chromosome 18 to one of three homologous genes at Xp11, SSX1, SSX2, and SSX4. Leiomyosarcomas have deeply eosinophilic cytoplasm, blunt-ended nuclei and juxtanuclear vacuoles. Deep-seated plexiform neurofibromas in the setting of NF1 that show high cellularity, diffuse cytologic atypia, and at least slightly increased mitotic activity may be diagnosed as low-grade MPNST arising in neurofibroma. Features favoring desmoplastic melanomas include dermal location in the head and neck region, junctional component, lymphoid response, and strong S-100 immunoreactivity. This image of MPNST shows round, oval, or spindle shaped hyperchromatic nuclei. The tumor cells have indistinct pale cytoplasm.



