Barrett Esophagus : Dysplasia Assessment

Comments:
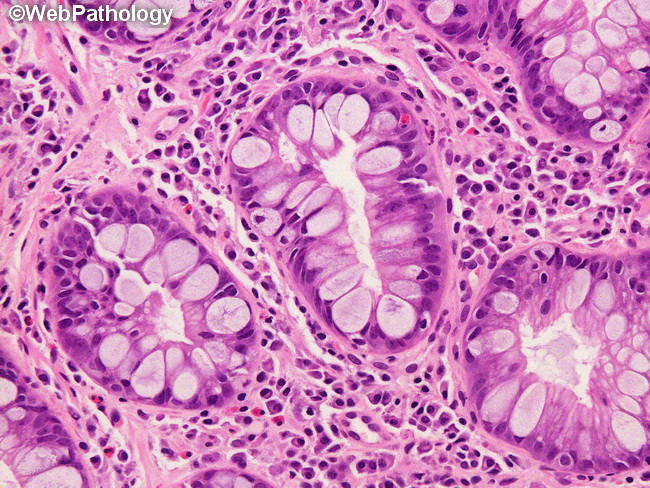
Assessment of dysplasia in Barrett esophagus (BE) requires evaluation of the following mucosal features: Surface maturation (best evaluated at low magnification): In the absence of dysplasia, the nuclei in the basal portions of the glands are larger, hyperchromatic, and more stratified than those in the surface glands. There is maturation towards the surface where the cells are arranged in a monolayer and have basally located small nuclei. Glandular architecture (best evaluated at low magnification): Normally, the glands are uniform, round, and surrounded by abundant lamina propria. Overcrowding of normal-appearing glands (back to back glands with little lamina propria) is a mild architectural abnormality. Glands with one or more of the following features are severely abnormal: variation in size and shapes, cribriform architecture, cystic dilation, and necrotic luminal debris. Cytologic features (best evaluated at high magnification): Mild nuclear enlargement and hyperchromasia is normally seen in the basal portions of the glands. These features disappear as the glands mature towards the surface. Cytologic atypia may be reactive (in the setting of inflammation) or caused by true dysplasia. Cytologic evaluation includes nuclear polarity. Normally, the nuclei of columnar cells are parallel to each other and their long axis is perpendicular to the basement membrane. When polarity is lost, the nuclei are arranged randomly with regards to one another and to the basement membrane. Inflammation, erosion, and ulcers: These are confounding factors which can cause cytologic atypia and make benign lesion look concerning for malignancy. Conversely, the inflammatory infiltrate can obscure a malignant lesion. The image shows Barrett mucosa with intestinal metaplasia. Image courtesy of: Phoenix Bell, MD.



