Malignant Mesothelioma : Differential Diagnosis

Comments:
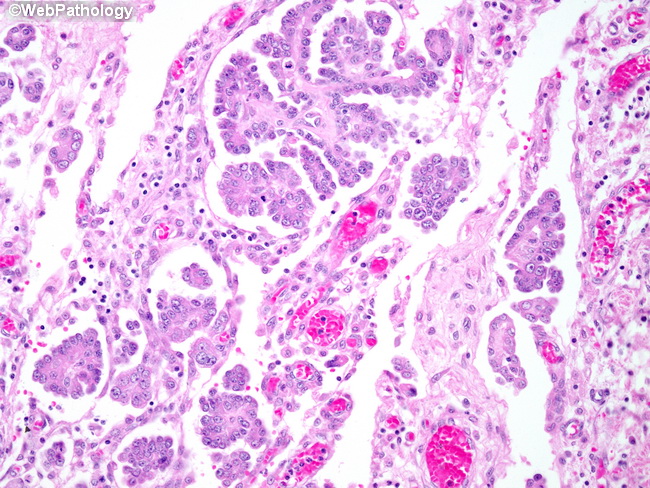
Malignant mesothelioma of the peritoneal cavity invading the serosal surface of the small bowel. The main differential diagnostic considerations are reactive mesothelial hyperplasia and papillary serous carcinoma (primary peritoneal origin or ovarian metastasis). The distinction between reactive mesothelial hyperplasia and malignant mesothelioma has been previously dealt with. Features favoring malignant mesothelioma over papillary serous carcinoma include: prominent tubulopapillary architecture, absence of significant nuclear anaplasia, absence of high mitotic rate, and the presence of abundant eosinophilic cytoplasm. The presence of intracytoplasmic mucin does not necessarily support the diagnosis of carcinoma as mucin-positivity has been documented in mesotheliomas as well. Immunohistochemically, positivity for podoplanin (D2-40), calretinin, and WT1 and negativity for Ber-EP4, B72.3, MOC-31, CA19-9, and Leu-M1 support the diagnosis of mesothelioma. If diagnostic ambiguity persists after immunohistochemical stains, electron microscopy can come to the rescue. Mesothelioma cells show long, slender microvilli coated with acid mucopolysaccharides and intracellular vacuoles.



