Myeloma : Bone Marrow

Comments:
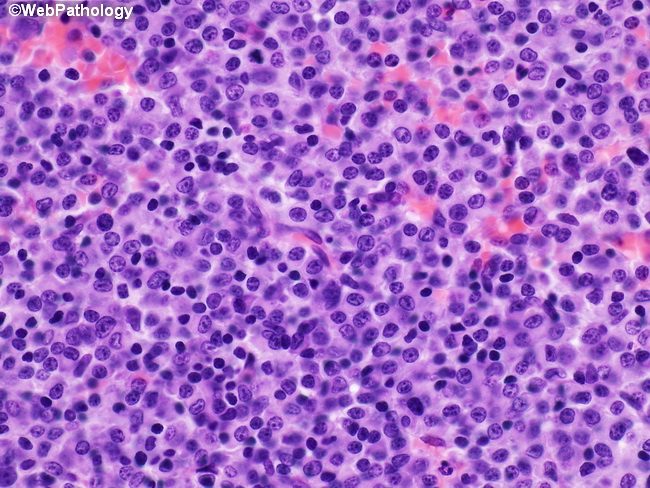
In multiple myeloma, the findings in bone marrow trephine biopsies can be variable and depend upon the tumor burden and stage of the disease. In early stages, there may be only focal lesions which may be distributed irregularly and missed on trephine biopsies. In advanced stages, the plasma cell infiltrates are diffuse and more readily detected. This case showed multiple focal lesions composed of immature appearing plasma cells (same case as the previous three images). The tumor cells have high nuclear-to-cytoplasmic ratio and dispersed chromatin. Some cells have prominent nucleoli. The islands of tumor cells are surrounded by normal hematopoiesis.



