Type A Thymoma : Differential

Comments:
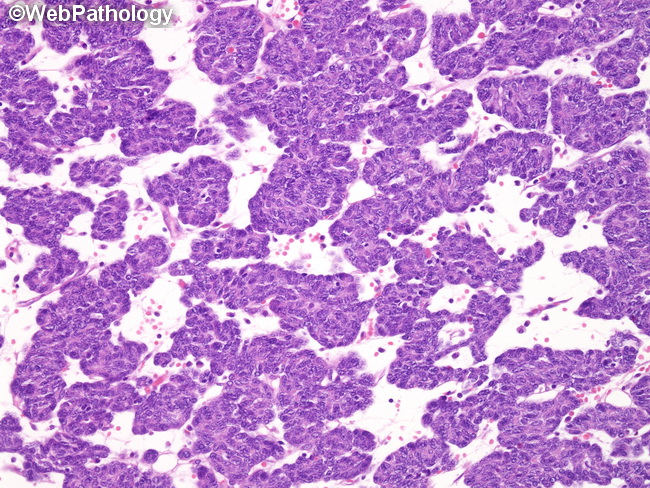
Type A thymoma needs to be distinguished from 1) Type AB thymoma: Type A thymomas have no or very few TdT+ immature thymocytes scattered among the spindle cells. By contrast, type AB thymoma has larger number of immature thymocytes. 2) Spindle cell variant of type B3 thymoma: Type B3 thymomas have prominent perivascular spaces � a feature seen less commonly in type A thymomas. In contrast, type A thymomas are more likely to show glandular structures, rosettes, and pericytomatous vascular pattern. 3) Thymic carcinoma: Although rare variants of type A thymomas may show cytologic atypia, increased mitotic activity, and even necrosis � these features are more likely to be seen in thymic carcinomas. Moreover, thymic carcinomas may show differentiation along the lines of squamous cell carcinoma, basaloid carcinoma, mucoepidermoid carcinoma, and lymphoepithelioma-like carcinoma among others. 4) Carcinoids and mesenchymal tumors: Given its spindle cell morphology, type A thymoma needs to be distinguished from carcinoids (that can show spindle cell pattern) and mesenchymal tumors that can arise in the mediastinum, including solitary fibrous tumor and synovial sarcoma. An immunohistochemical panel consisting of p63, CD34, STAT6, and CD56 can help resolve the diagnosis. This image shows a type A thymoma composed of bland spindle cells arranged in nests and trabeculae.



