Mucinous Carcinoma : Differential Diagnosis

Comments:
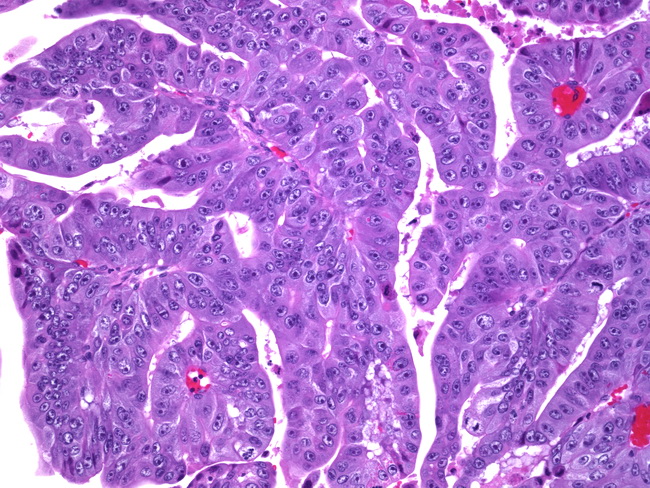
The differential diagnosis of mucinous carcinomas of the ovary includes: 1) Metastatic mucinous tumors of the ovary can clinically mimic primary ovarian mucinous neoplasms. The metastases usually originate from adenocarcinomas of large intestine, appendix, pancreas, biliary tract, stomach and cervix. Features favoring a primary ovarian mucinous carcinoma include unilateral involvement, expansile pattern of invasion, complex papillary architecture, presence of benign and/or borderline areas, and a large tumor size. Features favoring metastatic mucinous carcinoma include bilaterality, small size, multinodular growth, ovarian surface involvement, hilar involvement, extra-ovarian spread, pseudomyxoma peritonei, and signet ring-cell morphology. Most of the ovarian mucinous tumors associated with pseudomyxoma peritonei are metastases from low-grade appendiceal mucinous neoplasms. 2) Endometrioid carcinomas, Grade I, can show foci of mucinous metaplasia composed of benign endocervical-like glands. Some mucin-rich endometrioid carcinomas have glands distented with mucin. 3) Sertoli-Leydig cell tumors with heterologous elements can have a prominent mucinous component. It should also be remembered that some mucinous ovarian tumors can undergo stromal luteinization and produce virilizing symptoms which may lead to diagnostic confusion. Sertoli-Leydig cell tumors show sex cord-like structures in the fibrous septae. Other heterologous elements (like skeletal muscle or cartilage) may also be present and point to the correct diagnosis. The image shows expansile invasive pattern in a mucinous carcinoma of the ovary. There are crowded, back-to-back glands with little or no intervening stroma, creating a complex architectural appearance. There are no obvious areas of stromal invasion. The neoplastic cells show moderate to severe cytologic atypia.



